My Birth Experience with Theo | First Time Mom | Pregnancy Diary

It’s been a little over 2 months since I gave birth to Theo and I finally feel as though I have the time to share my birth experience.
My pregnancy was pretty smooth (read my trimester diaries here!) but I wish I could say the same about my birth experience! One of the big things my prenatal class and midwives talked about was a birth plan so we created a birth plan in our final weeks before our due date. It didn’t have much aside from these:
- Vaginal birth.
- An epidural at 7cm dilated.
- Dan to be the one to announce the sex (we opted not to find out about the sex throughout the pregnancy).
- Dan is to be the one to cut the umbilical cord.
- Dan to catch the baby, if possible.

Wednesday, November 1
I woke up at around 9 am. The day progressed normally, but I had trouble falling asleep so I was wide awake when I felt the urge to pee on Thursday morning around 2 am. After crawling back into bed, I told myself I needed to sleep.
Thursday, November 2
As I was trying to fall asleep, I noticed my back starting to ache and I couldn’t get into a comfortable position. As time passed, the ache started to increase. One couple in my prenatal class gave birth a week earlier and shared her experience; one of her early labour signs was a backache. Eventually, my back was so uncomfortable that I was folding over and that’s when Dan woke up. I told him that I think labour just started.
As my back ached progressed, I started to experience discomfort in my hips. We used the TENS machine for the maximum allotted time which got rid of my backache permanently, however, the discomfort in my hips was still persistent. It was NOT painful, but just a constant ache that bothered me.
We left a non-emergency voice message to the midwives at around 7 am and I received a call from them around 9 am to discuss the labour and my symptoms. My midwife said she’ll check in again at 5 pm.
As the day progressed, the ache in my hips did not go away and my contractions were still far apart. I remember my prenatal classes saying that early labour should be used to rest (sleep, watch movies, etc.) but I was in so much discomfort (again, not pain!) that I could not rest or relax. As someone who hates baths, I ended up asking Dan to fill the bathtub to help my discomfort since water therapy was brought up in the prenatal classes as a pain management. That day, I spent hours in and out of the tub, trying to nap in the tub and managing my contractions in the tub. When I was not in the tub, I walked around the house and massaged my hips to alleviate the discomfort.
At 5 pm, my midwife called. I told her that the hip discomfort had not gone away and I asked if I could get a morphine shot and gravel to help me sleep since I hadn’t slept since the night before. She asked when was the last time I peed to which I replied at 2 am and she said… “So, you have not peed for 16 hours?!”
Instantly, we knew something was wrong. Throughout the day, there were times when I tried to pee (ie. not hold my bladder) but nothing came out and I didn’t overthink it. She gave some tips on how I can release my bladder but unfortunately, nothing worked so we agreed to meet up at the hospital for me to get a catheter inserted and to get the morphine shot and gravel.
When we arrived at the hospital, the midwife did a routine check on the baby and then inserted the catheter. Instantly, I felt a huge release as my bladder emptied and the discomfort in my hips instantly went away as the bag was being filled (I filled up almost 1L!). Once she removed the catheter, I felt a huge gush of liquid coming out of me and my midwife confirmed that my water just broke (this was around 6 pm). She checked how dilated I was and much to our surprise, I was 3cm dilated!
My midwife gave me a morphine and gravel shot and given how quickly I dilated, there’s hope that we will be back in the hospital in less than 24 hours. We went home, and I crawled into bed at around 8 pm and fell asleep.
Friday, November 3
Again, I woke up at around 2 am due to the discomfort in my hips. Since we figured that it was my bladder causing me discomfort, I tried to use the toilet but to no avail. Dan ran the tub again and I went in and out for a few hours. I knew I needed a catheter again but I felt very bad at the idea of waking up my midwife at 4 am so I tried my best to wait for a more “reasonable” time to call.
At around 4:30 am, Dan called our midwife and she agreed to come to our home to insert a catheter in me. When she arrived and emptied my bladder, she rechecked my cervix and noted that I dilated to 4-5 cm which meant I could officially check into the hospital labour room or I could wait at home until I was further dilated. I opted to check into the hospital early and we checked in at 7 am.
After settling in the labour and delivery room, I sat on the labour ball (aka the bouncy ball) to help progress my labour and did figure 8s for a while. Almost instantly, my contractions got closer and more intense which was a sign that I was getting closer to active labour.
As my contractions were progressing, I opted to use the big bathtub in the room and we spent almost 2 hours in the tub. Ladies, water therapy TRULY helps and it helped even more during active labour!
At around 11:30 am, we discussed getting the epidural. At this point, I’ve dilated to 7cm and I’ve been using the laughing gas to help with the pain for the past hour or so. I knew that from this point on, I would get nervous about the contraction pains since they were longer and more intense so I opted to get the epidural.

I was starting to get hungry so we prepared some food when the anesthesiologist came in for the epidural… which meant I could no longer eat! I shoved a quick peanut butter cracker into my mouth as they were preparing the equipment.
The procedure to get an epidural scared me because all I could think about was the risk of paralysis. My midwife was walking me through the procedure and at first, I couldn’t get into the correct position until Dan described it as getting into a cat position (yoga). Once my position was satisfactory, the anesthesiologist cleaned my back, numbed me (just a quick pinch!), and located my epidural space… there was not enough space for the needle so they had to go one notch down! They mentioned when this happened, it’s usually the posture is super straight or perhaps a slight fusion in the area.
Instantly, I felt a cool sensation overtake my body and I was losing sensation in the lower half of my body.
From here on out, it was uneventful. Shortly after getting the epidural, I was given oxytocin to help with my labour because my cervix was ripening BUT we had concerns that the baby wasn’t dropping enough. This meant that my contractions were not strong enough to push the baby further down. Several hours after receiving oxytocin, and my charts showing that I was having increased, long, contractions, the baby was STILL not dropping far enough… so my midwife got me into an exaggerated side lying to help get the baby in position. After two hours of this exaggerated side lying, the hip discomfort returned, so we removed the ball between my legs. At this point, the midwife inserted a permanent catheter to reduce the risk of an infection if they kept inserting and removing a catheter. Unfortunately, the hip discomfort did not go away despite my bladder being empty so I increased the epidural a bit which helped.
Eventually, I was fully dilated to 10cm and it was time to push. I think this was around 10:00 pm or 10:30 pm. Since I received the epidural, it blocked the natural sensation to push so I had guided pushing and breath work. I pushed for an hour and my midwife could feel the baby descending but not enough. At this point, the hip discomfort came back and wouldn’t go away despite the increase in epidural – and since we had the catheter in me, we knew it wasn’t a bladder issue anymore. Despite the pain, we tried again for another 30 minutes but the pain and discomfort were getting too much, the baby wasn’t descending, and I was running out of energy since I hadn’t eaten all day.
The midwife was getting concerned because she believed it wasn’t in position. Still, she wanted a second option so we called the gynecologist (my delivery doctor) into the room for his assessment. He confirmed that the baby’s head was looking up and not tucked in so a cesarean was required to get him out. However, since there was no risk to the baby (or me) at this point, I was given the option to get the cesarean or wait a few more hours to see if the baby’s head would get into the correct position for it to descend. In his professional opinion, he did not believe the baby would descend, and my midwife has also noted that it’s been more than 12 hours since my water broke.

Saturday, November 4
After a few minutes of discussing this with Dan, we opted for the cesarean because we felt it was time for the baby to come out and we’ve been trying for hours with no improvement.
Almost instantly, they prepped me for surgery. I was given a shower cap and some socks and was told to remove all my jewellery and piercings. Once the OR was ready, they transferred me into the room with my midwife beside me. The anesthesiologist there began to increase my epidural and the other assistants started prepping me for the surgery by shaving and sterilizing the area. At this point, Dan was also invited into the OR.
My fear with a cesarean delivery was the epidural not working and feeling the pain. I remember feeling pricks and pokes early on which got me telling my midwife that I feel a blade across my stomach but they didn’t stop. It turns out, they have already cut into me and started the surgery.
To be honest, the surgery was much quicker than expected. I did not feel any blades but I felt pressure and tugging which was extremely unsettling and uncomfortable. All I could think about is, it’s almost over, it’s almost over. My midwife warned me that an intense pressure was coming my way which is exactly what happened – I couldn’t describe it but it felt like a 200lb person punched my chest and took my breath away. I didn’t make a sound throughout the surgery but the massive pressure made me yelp, which was also the final pressure of getting the baby out. Instantly, I felt relief and I heard the cries of my baby! I remember hearing the doctor telling Dan he could cut the umbilical cord. A few seconds later, someone shoved a phone in my face which had a picture of my baby and confirmation that it was a boy. Theo was officially born on Saturday, November 4th at 1:39 am, one day earlier than his due date, weighing 3.98 kg or 8.12 lbs.
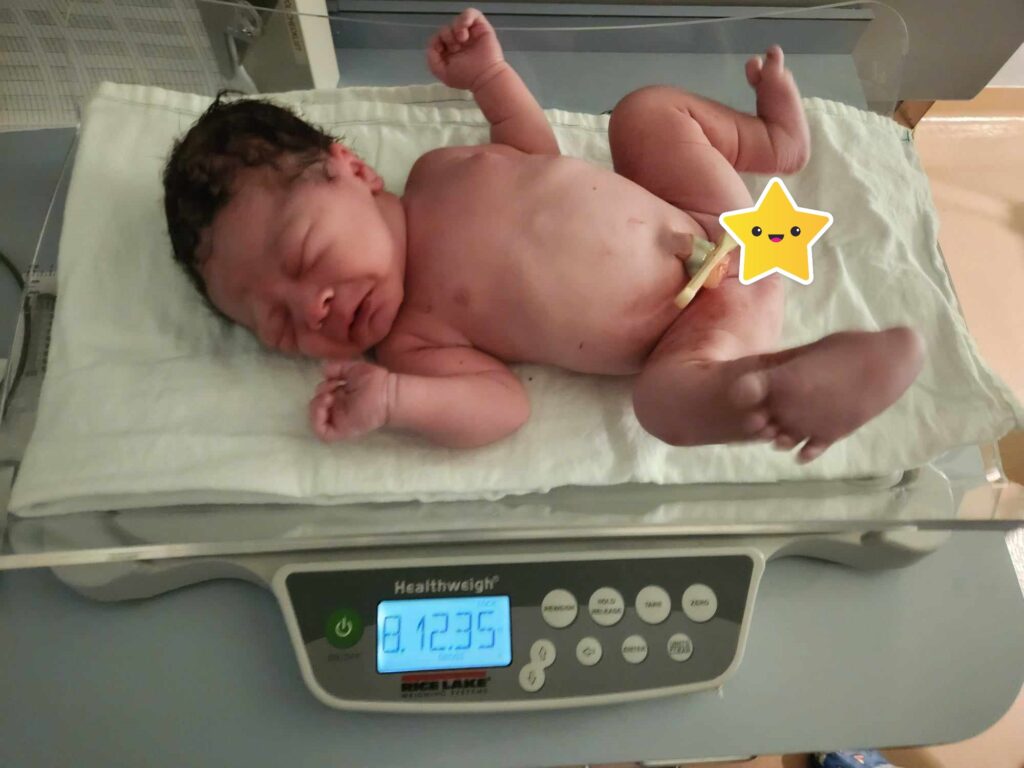

I think at this point, I was in shock from the ordeal. I heard my doctor saying something was wrong (the doctor knicked something so I had a pint of blood transfusion), so I asked the anesthesiologist how long would it take for them to sew me up and she replied, “About 20 minutes”. I begged her to put me under because I couldn’t take it anymore. She asked once more if I was positive I wanted to be put under and I said yes and started to count to 10. I woke up about 2 hours later and was reunited with Dan and Theo.

Despite our birth plan going out the window, it ended up being a good call to consent to the cesarean section. When our son was born, the doctor’s assessment was correct – his head was sideways and due to the 1.5 hours of pushing, his face was swollen when he came out. On top of that, we found a loose knot on the umbilical cord and the doctor theorized that if we had a vaginal birth, the knot could’ve tightened on the way down and risk losing oxygen to the baby. Ultimately, it was the right call to get a cesarean. The recovery process wasn’t too bad – I took my midwife’s advice and moved as much as I could which helped speed up the recovery. Looking back, the shock of the cesarean surgery led me to ask the anesthesiologist to put me under and I think if I had mentally prepared myself, I would’ve been awake from start to finish.












Congratulations on the birth of Theo! It was amazing to read your experiences, and even though things did not go completely as planned (or hoped for), it seems like you did a great job. I am wishing you all the best as you heal and spend time with your lovely baby. Congratulations again!
Congrats! I always find it strange how you can’t eat with an epidural as here in the UK we can and I was snacking when I had mine, until the gas and air made me sick! Sounds like a scary labour, mine didn’t go to plan either. But it just all happens so fast, doesn’t it?